As opioid deaths rose to a record high in 2020, researchers and clinicians across U-M kept up their effort to fight the opioid epidemic with data, evidence-based pain care and overdose prevention.

Eighteen months ago, COVID-19 grabbed the national spotlight from another major national health crisis — the opioid epidemic.
But that “other epidemic” hasn’t gone away, and in fact, has gotten worse. Annual opioid overdose deaths rose to a record high of more than 93,300 Americans in 2020. The COVID-19 and opioid crises have intertwined through forces such as social isolation and economic upheaval.
That’s why dozens of researchers and clinicians across U-M have kept up their effort to fight the opioid epidemic with data, evidence-based pain care and overdose prevention. They collaborate under the umbrella of U-M’s Opioid Solutions initiative, launched in 2018.
The Michigan Opioid Prescribing Engagement Network (Michigan OPEN) was launched in 2016 to respond to the mounting opioid epidemic in the state of Michigan. The network set out to address postoperative and acute care opioid prescribing, which at the time had little evidence to guide practice.
In this video, Michigan Medicine’s Dr. Michael Englesbe, professor of surgery, and Dr. Keith Kocher, associate professor of emergency medicine talk about the importance of the emergency room as an important care setting with opportunities to identify and curb opioid misuse.
Right-sizing opioid prescribing for acute pain
One of the biggest efforts at U-M addresses one of the “upstream” factors in the opioid epidemic: the overprescribing of opioid-based medications to treat acute pain after surgery or a dental procedure.
Such prescriptions have been seen as an important factor in the life trajectories of many people with opioid use disorder or overdose.
That’s why a U-M team launched a major effort to understand how surgeons, dentists and others prescribe opioids to ease their patients’ acute pain, how patients actually use the pills and capsules they receive, and what they do with the leftovers. Learn more about their recent findings here.

The team’s work has shown over-prescribing of opioids to patients who had many types of operations and procedures, as well as under-use of over-the-counter non-opioid pain relievers. Most troubling, multiple U-M studies have shown new persistent use of opioids among a minority of patients who received opioids — use that lasted months after the pain from their procedure should have faded.
The team, which calls itself the Michigan Opioid Prescribing Engagement Network, or Michigan OPEN, used these findings to create opioid-sparing pain care guides for surgeons, dentists and patients. They’ve studied the impact of these guides on prescribing patterns, and on patients’ pain and satisfaction with their care.
They’ve also organized community events, and helped organizations do the same, where members of the public can safely dispose of unneeded opioids.

Helping people with chronic pain get better care
Another U-M team is working to help those who have taken opioid-containing medications for years to ease the pain of chronic conditions, from lower back pain to complex pain syndromes. Such patients need special attention from their health providers, including help in accessing pain care alternatives that don’t carry the risks and side effects of long-term opioids. But U-M research has shown they often have trouble getting access to the care they need, because of a combination of stigma against opioid use, administrative hurdles and lack of resources at primary care and specialty care clinics. A recent IHPI brief summarizes this issue and lays out pathways to address it.
As the national legal settlement of court cases against prescription opioid manufacturers takes shape, IHPI experts have outlined ways some of the money could be used to improve pain treatment and address resource gaps for patients with acute and chronic pain.
Doctors may soon get more guidance from the CDC about prescribing opioids to people with chronic pain. Another IHPI team recently partnered with CDC experts to study the impact of the last CDC guideline for the use of opioids in chronic pain, issued in 2016. Read what they found here.
Treating opioid problems and preventing overdose
For people whose use of prescription and street opioids has escalated into problematic use — what lay people call addiction and what researchers call opioid use disorder — the need for solutions is urgent.
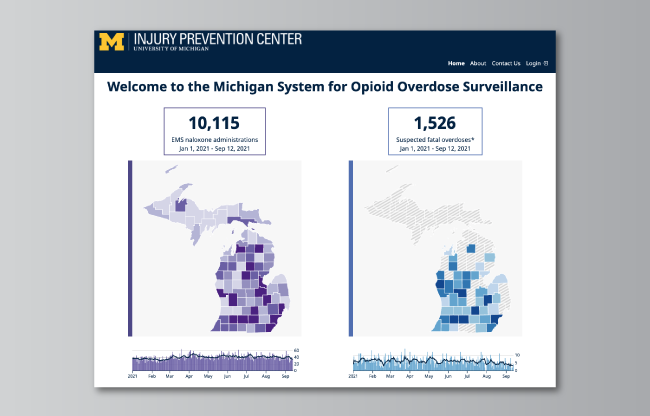
U-M teams are tackling this need on several fronts, including creating a real-time map of overdoses in Michigan by merging data from many sources in a way that can help health and law enforcement agencies focus their efforts.
They’re also working to get more people into outpatient treatment with the medication buprenorphine, which can smooth the transition away from problematic use of opioids. The rise of insurance coverage for telemedicine, and the relaxation of federal rules around buprenorphine prescribing, could help, as IHPI experts discuss here.
Another major effort underway involves naloxone, a medication that can reverse an opioid overdose if given in time. IHPI teams are working to study the patterns of naloxone prescribing, and to help emergency departments give naloxone kits to at-risk patients before they leave.
